Medically Reviewed by Kimberly Langdon, M.D.
If you have a loved one admitted to the hospital for intensive care attention due to a critical illness, chances are high that you will not be at rest. You will feel challenged, fearful, out of your comfort zone, stressed, vulnerable, stressed and overwhelmed. In addition to this, you may even feel handicapped because other people are running the show in this rather complex situation.
How long does it take to wean off a ventilator?
One question that hangs on the minds of those whose loved ones are in the intensive care unit of a hospital is that of “How long does it take to wean off a ventilator?” it depends, it can take between a few days to some weeks and even months. This is however largely dependent on the criticality of the patient’s condition. If however, it appears like it is taking too long, you may want to consider some viable alternatives.
The Different Stages And Time Frame For Ventilator Use
As far as the use of a ventilator is concerned, there are different timelines for different categories of patients. The nature of the admission and underlying medical conditions of the patient also plays a vital role in this regard. Here are some of the stages and time frames you should know about.
1. Soft and Straightforward admissions
If your loved one is a direct admission to intensive care after planned or elective surgery, they should be able to come out of the respirator/ventilator and out of the induced coma in about three days at the most, but it really depends on the underlying health of the person.
Breathing tubes and ventilation after surgery are carried out as measures to stabilize and ensure that the patient is oxygenating and meeting parameters ensuring that they can breathe on their own before they are taken off the respirator/ventilator. This is usually very important especially after surgery.
This is also applicable to some other soft admissions that are made into the intensive care section after a loved one may have developed some breathing associated issues and may need a respirator/ventilator for some time. This is to allow the lungs to clear fluid and secretions by using extra oxygen and air pressure to open the small air sacs called alveoli.
2. Ventilation for three to seven days
If the critically ill patient is in a rather complicated admission to the intensive care and appears to be unstable, the ventilator may be needed for more than 72 hours. It is however noteworthy that being weaned off a ventilator after 72 hours is a bit more difficult because the longer ventilation pressures and controlled breathing make the risk of complications higher.
Therefore, if a patient that is critically ill is stable and has the strength to breathe on their own, then there is no reason why they can’t be taken off the ventilator after about a week. It, however, depends on whether their chest X-Ray is clear, if they are oxygenating their blood and vital organs, and if they can breathe by themselves with little support from the respirator/ventilator.
3. Ventilation for more than a week
If your critically ill loved one has found themselves in the intensive care unit for over a week and has been under ventilation for over seven days, you may be worried. In a case where the intensive care team does not feel confident enough to remove the breathing tube after about a week, they may recommend a tracheostomy.
However, before they can suggest a tracheostomy, they should attempt to remove the patient from the induced coma first and if the patient is waking up and cooperating, the team should remove the tube. After removing the tube, they should try and find out if the patient can breathe comfortably without the use of the tube.
If this however fails, the team may then recommend a tracheostomy. This however, should not be an option until about 10 days of ventilation with a breathing tube has elapsed. It should also only be considered when the intensive care team is sure that there is no other viable alternative.
In addition to this, as far as tracheostomy is concerned in America, the inherent risk lies in the fact that the moment a tracheostomy is carried out, the ICU would want to send the patient to long-term assisted care. This may not be the desired outcome because LTAC is made in such a way as to cut costs and provide care of less acuity.
It, therefore, suffices to say that when LTAC becomes an option before or after the tracheostomy, you should ask a lot of questions to see if your loved one can be offered alternatives. However, LTAC may be the only option for someone who is healing slowly.
The only reasonable option for patients on ventilation alongside tracheostomy is intensive care at home. In this situation, highly professional and skilled intensive care nurses will provide the needed care in your home for the patient as a viable alternative to the intensive care unit of the hospital.
What Are The Important Things To Be Mindful Of When Having A Tracheotomy?
Tracheostomy is considered when the critically ill patient has gone through a series of failed extubations and is unable to breathe without the aid of a ventilator. In addition to this is the fact that the critically ill patient may need to remain in intensive care for longer periods using ventilator support.
The advantage of a tracheostomy is that the critically ill patient can be removed from the induced coma and would be able to wake up and communicate. This may, however, be non-verbally as it does not give the patient the ability to talk.
Have it at the back of your mind that with ventilation using breathing tubes in the mouth, it would be necessary for an induced coma. However, a tracheostomy is more tolerable because there is no need for an induced coma. Furthermore, a tracheostomy also has the added advantage of removing your loved ones from the ventilator quicker by attempting to breathe without the ventilator just through the oxygen mask using humidified oxygen through the tracheostomy. The longer a person is on a ventilator, the weaker their chest wall muscles become, which makes weaning from the ventilator harder.
The aim is to improve the frequency which the patient can stay without the respirator/ventilator. This may initially be two hours on the ventilator and two hours off of it. The moment the patient can stay without the ventilator for over 24 hours, they would be able to leave the intensive care unit even while the tracheostomy is in place. However, most patients should be able to get the tracheostomy removed while they are in the intensive care unit before they go to the ward. This involves closing off the tracheostomy for extended periods of time to see if the patient can mouth of nose breathe.
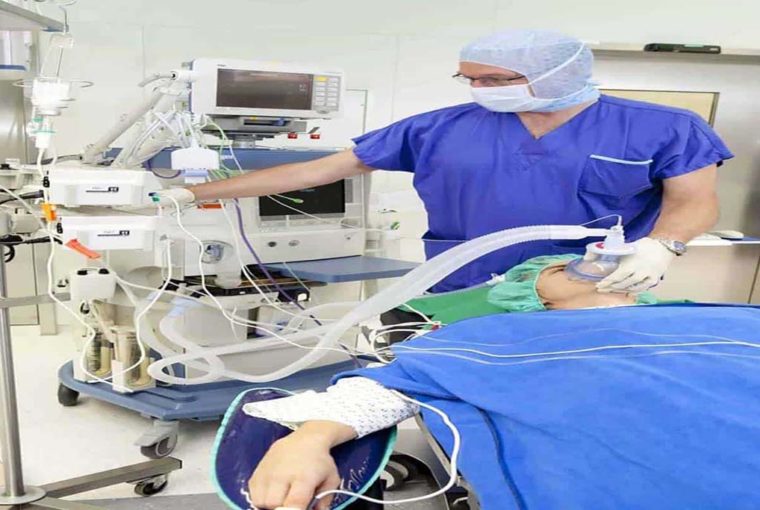
What Exactly Is A Ventilator And How Does It Work?
A ventilator is simply a machine that assists people with breathing when they are unable to do that on their own. It supports the breathing of the patient while the body heals from surgery or other medical conditions such as pneumonia. The doctors will attempt to get the patient off the ventilator at the earliest possible time.
The ventilator works either by doing the breathing or assisting the patient with the breathing. For this to be achieved, the doctor sedates the patient using drugs upon which he introduces the tube known as the endotracheal tube (ET) via the mouth into the trachea. Mucus secretions can be cleared through suctioning out via the ET tube. This tube is linked to the ventilator.
If the ventilation is to be prolonged, a decision may be made to carry out tracheostomy. This is a situation where the doctor creates an opening in the neck of the patient and places in a tube which is then linked to the ventilator that provides oxygen and removes carbon dioxide from the lungs.
How Does A Patient Feel When They Are On The Ventilator?
The feeling the tube creates when in the mouth can be quite uncomfortable. This is because the test tube goes through the vocal cords which means they will not be able to speak. A lot of patients find this rather frustrating. They won’t be able to drink or eat, however, teeth cleaning and mouth care can be carried out by staff.
The patients can, however, be fed using tubes that go through their stomach through the nose. To increase comfort, a continuous drip of sedating drugs will be passed through the IV. When improvement is observed in the patient, the tube will be removed while an oxygen mask is used instead. This usually takes between a few hours to some weeks.
How Is The Progress Of The Patient Monitored?
Patients admitted to the intensive care unit are regularly observed to measure their heart rate, blood pressure, oxygen levels, and temperature. Other tests carried out include measuring the carbon dioxide and oxygen levels via a blood test. This is regularly reviewed by the ICU staff. When the patient wakes up, they are reassured and made to understand where they are and why.
What Are The Risks That Come With Ventilation?
One of the major challenges of ventilation is an infection. Even though there are several ways to lower the risk of infection like mouth care and removing the mucus by suctioning, the ET tubes can permit germs to find their way into the lungs which may then lead to an infection of the chest. This may delay the progress of the patient thus extending their time on the ventilator.
What Does Weaning From A Ventilator Mean?
This simply means lowering the ventilator support which may be carried out rather quickly or gradual in other cases. This is usually more difficult for the patient when they have been on the ventilator for a while.
Conclusion
How long does it take to wean off a ventilator? The time frame is largely dependent on the state of the patient and their medical condition. It could take between days and weeks as the case may be.
You may like these articles as well:
Can Diabetics Drink Coke Zero?
Is Aids An Autoimmune Disease?
How To Starve Your Body To Lose Weight?